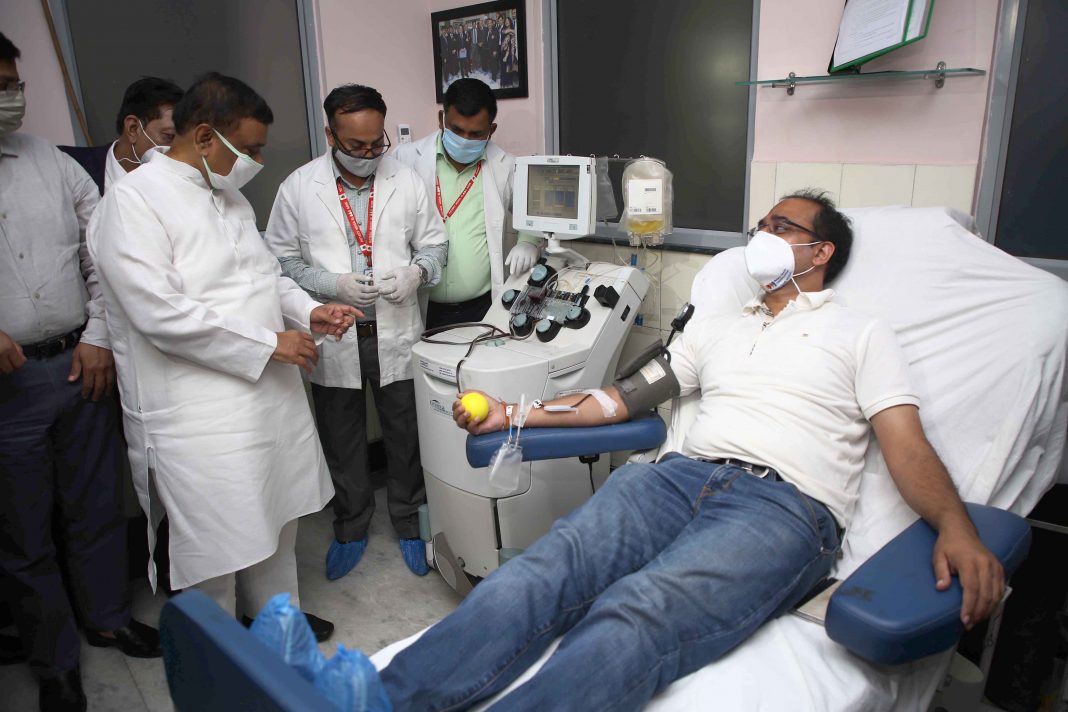
There has been much debate about the pros and cons of the therapy and trials have shown that it improves symptoms like difficulty in breathing and fatigue. But the decision is best left to the physician.
By Dr KK Aggarwal
The severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), which causes Covid-19, is proving to be a mysterious virus even though knowledge about the disease is evolving every day. Accordingly, the guidelines for the management of patients are developed and regularly updated, based on the latest research. This has created several challenges, one being the discrepancy between trial findings and their clinical application.
There were no specific drugs for the treatment of Covid-19 till now and drugs were being repurposed as potential treatment for the disease. However, the multi-country Solidarity Therapeutic Trial, spearheaded by WHO, found that remdesivir had no effect on mortality in hospitalised patients with Covid-19. The other drugs tested alongside were hydroxychloroquine, lopinavir/ritonavir and interferon, but they also did not reduce mortality. The results were surprising as trials by the National Institute of Allergy and Infectious Diseases, published on October 8, 2020, in the New England Journal of Medicine had shown that recovery was faster with remdesivir in hospitalised patients with Covid-19. On October 22, remdesivir became the first treatment for Covid-19 to receive FDA approval for use in adults and children aged 12 years or older.
Another line of treatment is convalescent plasma, which is experimental, and has received regulatory approval for its use in Covid-19 patients who do not respond to standard treatment. It was accorded emergency use authorisation by the FDA as a potential promising treatment.
Convalescent plasma is plasma collected from persons who have recovered from Covid-19 by the process of apheresis. This is a medical procedure where whole blood is removed from a donor or patient and separated into individual components so that only one component can be removed. Plasma therapy has been used as an emergency intervention in many outbreaks, including the Spanish Flu, SARS, MERS and Ebola. Except for Ebola, it has been beneficial when administered early in the course of the disease.
Read Also: Supreme Court grants custody of child to the mother, allows the father visitation rights
Convalescent plasma contains protective, neutralising antibodies to the coronavirus. When transfused into a patient, these antibodies have a direct antiviral action by suppressing virus replication and may hasten recovery. The presence of anti-inflammatory cytokines, clotting factors, natural antibodies and other undefined proteins in the plasma may further enhance anti-inflammatory and immune modulatory response. Convalescent plasma can be collected anytime between 14 and 28 days following Covid-19. Anyone who has recovered from Covid-19 and completed 28 days after the completion of treatment or home isolation and is between 18 to 60 years is eligible to donate their blood plasma.
According to the Delhi Plasma Bank website, the potential donor must have had documented Covid-19 infection and tested negative for the virus. These guidelines also specify that persons weighing less than 50 kg, diabetics on insulin, persons with uncontrolled diabetes or hypertension with change in medication in the last 28 days or persons with kidney/heart/lung or liver disease, cancer survivors or persons with systolic BP more than 140 and diastolic less than 60 or more than 90 are ineligible for convalescent plasma donation.
Women who have been pregnant also cannot donate plasma. This is because pregnant women develop anti-human leukocyte antigens (HLA) antibodies against paternal antigens. These anti-HLA antibodies usually have no effect on the woman or on her subsequent pregnancies. But when plasma containing HLA antibodies is transfused to a person with lung damage, as generally occurs in Covid-19, this may lead to transfusion related acute lung injury (TRALI), a potentially life threatening condition. In countries like the US, such women are tested for anti-HLA antibodies before they can donate plasma.
The other standard eligibility guidelines for blood donation blood group, Rh and HLA typing, screening for blood-borne pathogens like hepatitis B and C, HIV also apply to convalescent plasma donation. The immune response to Covid-19 differs in different patients. Therefore, all convalescent plasma does not contain the same amount of antibodies and so are not equally effective. Other adverse effects include allergic/ anaphylactic reactions, risk for transmission of blood-borne infections, TRALI, transfusion associated circulatory overload and febrile non-hemolytic and hemolytic transfusion reactions.
Covid-19 induces a hyper-coagulable state in the body. Plasma contains pro-coagulants and hence must be used with caution in patients with acute thrombotic events, including older patients, those with cardiovascular risk factors and those with hyper-coagulable conditions such as inflammatory bowel disease.
Use of convalescent plasma as a treatment for Covid-19 is authorised for off label use in India. Delhi was the first state to use convalescent plasma as treatment for Covid-19. The country’s first convalescent plasma bank was also set up in Delhi in July.
The clinical management protocol for Covid-19, which was issued by the health ministry on July 3 includes convalescent plasma as an investigational therapy “for consideration in patients with moderate disease who are not improving (oxygen requirement is progressively increasing) despite use of steroids”. The dose ranges from 4 to 13 ml/kg (usually 200 ml single dose given slowly over not less than two hours). As per the ministry guidelines, certain prerequisites must be met before proceeding with the transfusion.
These include:
- ABO compatibility and cross matching of the donor plasma
- Neutralising titer of donor plasma should be above the specific threshold
- Recipient should be closely monitored for several hours post transfusion for any transfusion related adverse events
- Use should be avoided in patients with IgA deficiency or immunoglobulin allergy.
The effectiveness of convalescent plasma came into question following publishing of the PLACID (PLAsma Convalescent InDia) trial by the ICMR. It is the first randomised controlled trial in the world and was evaluated for safety and effectiveness. The trial was conducted in 39 hospitals, both public and private, across India on 464 adults 18 years and above with confirmed, moderate Covid-19. The results showed that while it was safe, there was no survival benefit of convalescent plasma over the best standard of care. However, the trial did show that plasma therapy improved symptoms like difficulty in breathing and fatigue with faster virus clearance.
So was the lack of survival benefit due to the fact that a majority of the donors in the study had mild disease and were young and fit? An editorial published on October 22 in The British Medical Journal has recommended that “only donor plasma with detectable titers of neutralising antibodies should be given to trial participants, to ensure that the potential for benefit exists for all intervention arm patients”.
Read Also: Bihar polls phase 1: Candidates with criminal records still rule the roost
Clinical practice today is undergoing a shift from evidence based medicine to personcentric or patient centric care. The Institute of Medicine has defined patient centered care as: “Providing care that is respectful of, and responsive to, individual patient preferences, needs and values, and ensuring that patient values guide all clinical decisions.”
Person centric medicine recognises that every person has a distinct set of characteristics that distinguishes them from the other. Every patient has to be managed differently for the best possible outcome. Individual response to drugs may vary, the side effects may vary. Treatment has to be tailored to each patient taking into consideration their individual characteristics, culture, personal preferences, expectations, etc. All these variables need to be taken into account when formulating a treatment plan for the best response and maximum safety of that patient.
New research and guidelines are suggestions and recommendations, which are definitely evidence based. While they do standardise treatment for any given condition, they are not without limitations. They cannot be generalised and extrapolated to all patients alike as each patient is unique and hence, treatment has to be individualised.
The first Covid-19 patient in the country to receive convalescent plasma therapy was given this treatment on compassionate grounds upon request from his family when there was no improvement with standard treatment. If trials and /or guidelines “dictate” or “decide” treatment, this impinges on the professional autonomy of a doctor. The decision to use a particular treatment modality and when to use it is best left to the treating clinician.
—The writer is President, Confederation of Medical Associations in Asia and Oceania, and former National President, IMA
Lead Picture: UNI